Minimizing hospital infections starts in the restroom
by Mark Lawinger

All images courtesy Sloan Valve Company
The transmission of infectious disease is a growing epidemic in healthcare facilities. Not only do these environments house people with weakened immune systems, but they also often serve as breeding grounds for disease-causing pathogens, thereby increasing the risk of patients contracting new illnesses.
Healthcare-acquired infections (HAIs) occur in every type of healthcare facility and can be spread in various ways—from direct contact with medical workers or other patients to ingesting or inhaling infected water or water vapor. These infections are caused by a number of microorganisms, including bacteria, fungi, and viruses. Studies have also shown almost half of all HAIs may be caused by infected water, while the other half can simply be a factor of unwittingly coming into contact with contaminated fixtures and surfaces. Hospital water systems and bathrooms can be ideal places for germs to breed. Many bacteria thrive between 25 and 42 C (77 and 108 F), the precise temperature range of most hospital water.
However, through smart restroom design and strategic specification of fixtures (e.g. faucets, sinks, flushometers, toilets, and urinals), healthcare facilities can minimize the spread of infection-causing pathogens. By implementing antimicrobial coatings and hands-free fixture operations, proper plumbing design can help prevent the spread of harmful germs and aid patient recovery.
Restroom fixtures fight back
If one sets foot in a doctor’s office waiting room containing 25 other people, statistics show someone in the room has acquired an HAI. According to studies conducted by the Centers for Disease Control and Prevention (CDC), U.S. hospitals report 1.7 million HAIs each year with an alarming 99,000 deaths resulting from infection acquired during hospitalization. Aside from the lost lives, HAIs cost hospitals $20 billion annually. Medical facilities literally cannot afford for these infections to continue plaguing patients.
Everyone knows practicing good hygiene is of the utmost importance in preventing the spread of germs. Users need to make sure they washed their hands in the cleanest environment possible. This is where restroom fixtures enter the conversation.
In restrooms with manual faucets, handles serve as a breeding ground for germs. Touching faucet handles after washing simply re-contaminates hands and may negate the benefits of cleaning them. While some experts recommend restroom visitors use a paper towel to turn faucets off, in reality, users are either unaware of this advice or choose not to follow it.

However, electronic, touch-free faucets make this a moot point because sensors are employed to activate and shut off the flow of water. The absence of handles removes a contact point for spreading dirt or harmful bacteria from one user to the next. Hands-free operation also allows the faucets to be used by anyone, regardless of age or physical ability. Another advantage is water conservation, as sensor-activated faucets can save water by running only when the user is actively wetting or rinsing hands.
Most electronic faucets rely on an infrared sensor. Once the user enters the sensor’s effective range, the solenoid activates the water flow. Tempered water flows from the faucet until hands move away. The circuit then automatically resets and is ready for the next use. Touchless faucets are often designed to operate for a preset amount of time when a user’s hands are in the active area. This type of faucet uses approximately 3.8 L (1 gal) less water per activation than a manual faucet.
Making alternate design decisions
Aside from how they operate, there are several other design considerations when specifying faucets in a healthcare environment. Sinks should be designed with one goal in mind—to get water down the drain quickly with as little splashing as possible.

While automatic faucet flush features avoid stagnant water in pipes, the optional LCD displays can guide users through handwashing recommendations. Additionally, gooseneck spouts allow handwashing up to the elbows and laminar flow faucets keep water from mixing with germ-filled air. In the case of laminar flow faucets, their spray heads provide a single, non-aerated, non-splashing stream, while a ‘multilaminar’ spray head—recommended for use in public restrooms—can be employed to produce a miniature shower pattern to provide full, non-splashing coverage of hands during washing. The Rush University Medical Center in Chicago specified faucets with a laminar flow to prevent drawing air into the water stream and, in turn, stop the introduction of bacteria contained in room air, keeping patients as free from bacteria as possible.
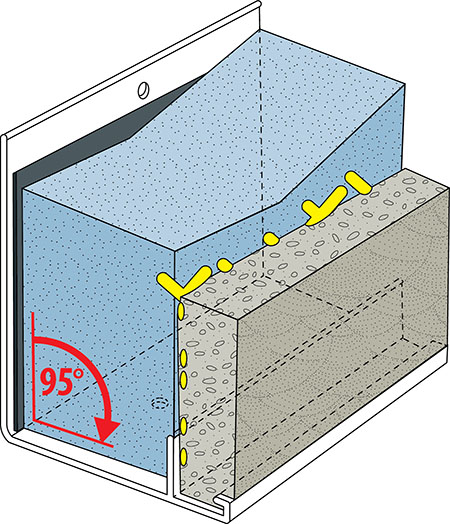
Hospitals require several types of sinks for specialized applications, but their design goals are similar. A sink basin should be deep enough to prevent water—and the bacteria living in it—from splashing over the sides. The faucet should be oriented so water falls on the ‘sweet spot’—the gently sloping portion of the sink, which encourages water to flow toward the drain. If the stream hits the drain directly, it can cause the splashing of potentially contaminated water.
To meet the goals of durability and sanitation, the best materials for most healthcare sinks include high-quality vitreous china, stainless steel, and solid surface. Antimicrobial coatings can be applied to surfaces to keep germ growth under control.
Limiting the damage
Flushometers, toilets, and urinals in healthcare facilities are obvious breeding sites for germs. However, smart specifications can mean less contact between germs and people. Wall-mounted toilets make floor cleaning faster and more effective. Vitreous china toilets and urinals can be treated with hydrophobic (water-repellent) and oleophobic (oil-repellent) properties to impact a fixture’s surface at a nanoscale. This makes the fixture easier to maintain and keeps it cleaner longer.
Touchless sensor flushometers inherently reduce germ-spreading contact and also serve an additional purpose of preserving water. Sensor flushometers are now reducing water volume by 30 percent and utilizing novel approaches such as dual-flush technology. These flushometers automatically use the proper volume of water for the type of waste being removed by initiating an amount of 4 L (1.1 gal) per flush (i.e. Lpf/gpf) or 6 Lpf (1.6 gpf) based on how long the user remains in the sensor range. This not only saves water, but is more efficient at keeping drain lines clean.
Another consideration for healthcare facilities is to implement bedpan washers into toilets to minimize the backsplash of infected water when nurses and hospital staff begin cleaning. The last place one would expect an HAI to originate is from a healthcare professional, but the unwanted backsplash from cleaning bedpans often puts staff in direct contact with bacteria. Facilities such as Elmhurst Hospital in Illinois have utilized this tactic to give nurses a more efficient way to clean bedpans. The washing system also eliminates the need for unsanitary hose sprays, which require extra housekeeping and pose a slippage danger to patients. Rush University Medical Center also utilized this approach to not only reduce the splashing by the bedpan washer, but also saves water.
Conclusion

Unfortunately, there is no magic wand anyone can wave to completely eliminate HAIs from hospital environments. The fact is a growing number of viral infections and bacterial strains continue to plague healthcare facilities across the world. However, by making responsible decisions about handwashing and specifying restroom products that lend themselves to a sanitary environment, hospitals can start to significantly cut down on facility inflicted illness and death as well as boost their bottom line in the process.
 Mark Lawinger has been the fixtures product line manager for Sloan for more than seven years and focuses on the healthcare market. He has a background in business development, marketing, and product management for commercial and industrial systems. Lawinger can be reached at mark.lawinger@sloanvalve.com.
Mark Lawinger has been the fixtures product line manager for Sloan for more than seven years and focuses on the healthcare market. He has a background in business development, marketing, and product management for commercial and industrial systems. Lawinger can be reached at mark.lawinger@sloanvalve.com.