Specifying windows for behavioral healthcare projects
Connect to the environment
Daylight and outside views, thermal and acoustic performance, and recycled composition of windows’ materials can aid buildings’ certification efforts under such programs as LEED. Since its inception in 2000, U.S. Green Building Council’s (USGBC’s) voluntary, consensus-based LEED rating system has emerged as the leading sustainable building “scorecard.”

Photo © Marilyn Ott-Close/courtesy Apogee Architectural Metals
Currently, LEED Building Design and Construction (BD+C) or LEED for Operations and Maintenance (O+M) both apply to healthcare facilities seeing certification. As of March 2025, there were 3,981 LEED‐certified and -registered healthcare projects worldwide, representing approximately 84 million m2 (904 million sf) of built space. Of these, 38 U.S. healthcare projects were LEED-certified in 2024, covering 6.3 million gross square feet. California had the most LEED-certified healthcare facilities in 2024 with 11 projects, followed by Texas with seven.
Other healthcare organizations may specify projects meet LEED criteria, but do not have to pursue certification. For example, the VA sustainability guidelines for facility construction and renovation projects require designing a project to meet LEED Silver certification or higher.
Environmentally responsible design and operation is a top-of-mind issue for anyone in architecture, construction, and real estate. Buildings represent about one-third of the energy consumption in the United States, along with the corresponding amount of greenhouse gas (GHG) emissions.
According to the National Academy of Medicine (NAM), “The health sector is a key contributor to climate change, generating 4.4 percent of carbon emissions globally and 8.5 percent of emissions in the United States.”
A question of economics?

Photo courtesy Apogee Architectural Metals
In 2011, an “Economics, Efficiency, Energy & Environment” survey was conducted by the Corporate Reality, Design, and Management Institute (CRDMI) in partnership with the Healthcare Council of the International Facilities Management Association (IFMA). Many of the 1251 respondents—architects, designers, engineers, hospital facilities managers, healthcare engineers, project managers, and contractors—underestimated the impact design and operations could have on a hospital’s financial health. The survey summary notes:
Given a 4 percent total margin, saving $1 in energy equals $25 in revenue, and for the average-sized hospital in the U.S. that translates to an additional $7.2 million in revenue.
Less than 15 percent of the 2011 survey respondents said they select products or equipment based on durability and expected lifecycle. Today, products’ material composition and longevity are increasingly under evaluation, including by programs such as the LEED and the International WELL Building Standard. Environmental Product Declarations (EPDs), Health Product Declarations (HPDs), Declare Label as Living Building Challenge Red List Free, and other supporting documentation assist specification and design professions with evaluation and selection.
By keeping any claims and representations focused on tested, third-party validated, performance parameters, as well as sound engineering judgment, manufacturers can present a credible case for their products’ support of sustainable design initiatives.
In Washington, D.C., Saint Elizabeths provides intensive, in-patient care for individuals with serious and persistent mental illness. (Under the aforementioned survey, only three percent of respondents from D.C. indicated sustainability features took precedence in the final selection of their last building project. Half of these participants also said LEED certification, or the U.S. Environmental Protection Agency’s [EPA’s] Energy Star for Buildings program would be the most important next step in pursuing sustainability goals.)
Established in 1852, Saint Elizabeths Hospital was the first large-scale, federally run hospital for people with mental illness. Its design incorporates numerous sustainable design elements emphasizing daylighting and external views. Patient safety and security remained a top priority. Windows were furnished with interior polycarbonate glazing for human impact resistance. The move into a new facility completed a transition from the historic, psychiatric institution into a modern, healing environment.
Conclusion
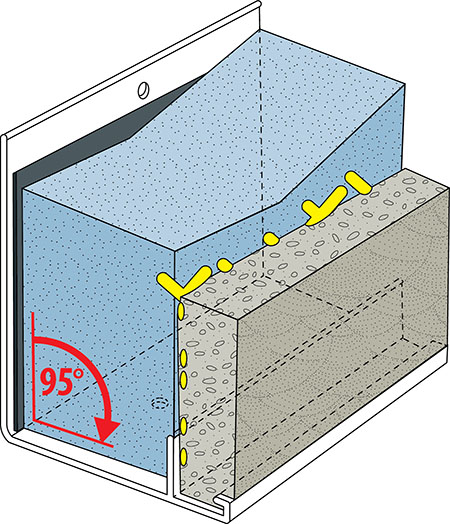
Whether building a new hospital, renovating existing spaces, or leveraging adaptive reuse of areas originally intended for another occupancy, window selection in areas accessible to psychiatric patients can be very challenging. Windows without jail-like bars or heavy security screens help create a more home-like and caring atmosphere with unrestricted views to the outside. At the same time, patient safety must remain the primary consideration.
Through development programs with state agencies and their architectural consulting partners, leading window manufacturers have designed psychiatric-grade fenestration systems answering this need.
Lisa May is the director of preconstruction and architectural services with Apogee Architectural Metals segment, providing technical assistance, sustainable design input, thermal modeling, detailing, and specification review to design professionals nationwide. She successfully completed Six Sigma training and the U.S. Green Building Council’s (USGBC’s) Leadership in Energy and Environmental Design (LEED) Green Associate accreditation. May instructs others in American Institute of Architects/Construction Specifications Institute (AIA/CSI)-approved continuing education programs addressing thermal and acoustical performance, and window and curtain wall selection. She can be contacted via email at lmay@apog.com.